Regulating the Nervous System Beyond Words
Trauma lives in both memory and physiology. Integrative posttrauma therapy recognizes that healing must address thoughts and emotions, but also the body, the nervous system, and the deeper regulatory systems that shape survival responses. True transformation involves more than symptom stabilization; it requires restoring balance to the stress response, supporting cellular energy production, and helping the body relearn safety.
Within this broader integrative framework, energy medicine offers a set of noninvasive tools designed to support self-regulation and nervous system recalibration. While the term “energy” can sound abstract, many forms of energy medicine rely on measurable physiological mechanisms—electrical microcurrents, light frequencies, electromagnetic fields—that influence neural signaling, mitochondrial function, and neurotransmitter activity.
Rather than replacing psychotherapy, these approaches enhance it. They create conditions in which emotional processing becomes more accessible, less overwhelming, and more sustainable.
What Is Energy Medicine?
Energy medicine refers to therapeutic approaches that work with the body’s electrical and physiological signaling systems to restore regulation. The term “energy” in this context does not refer to spirituality, mysticism, or abstract forces. It refers to measurable biological processes.
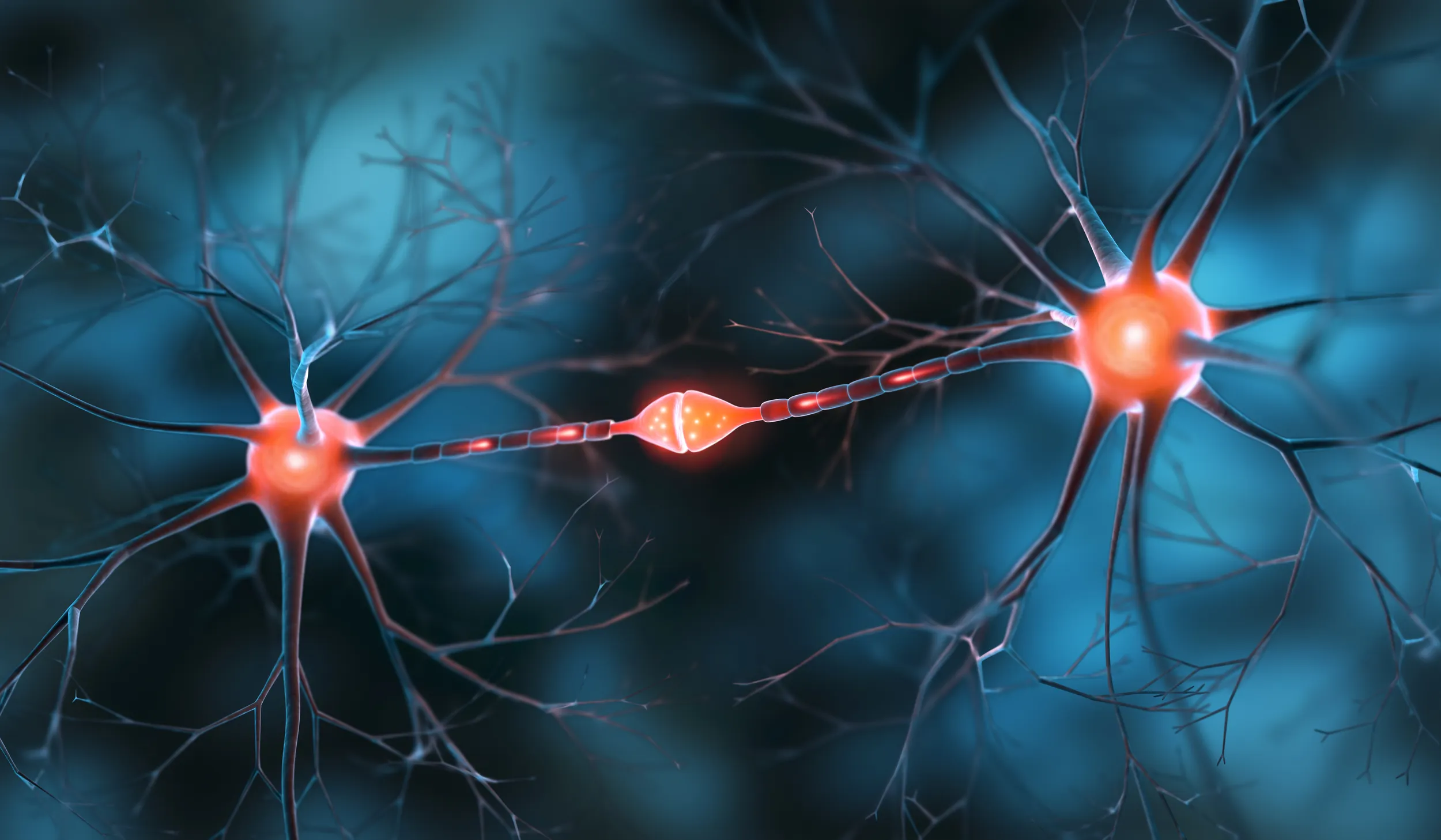
The human nervous system functions through bioelectrical signaling—neurons communicate via electrical impulses, the heart maintains rhythmic electrical patterns, and every cell depends on membrane voltage gradients to function properly. Light, sound, and electromagnetic frequencies are also forms of energy used routinely in conventional medicine, such as in ultrasound or laser therapies for pain and tissue repair. These are not esoteric concepts; they are foundational principles of physiology.
Trauma can disrupt these regulatory systems, contributing to autonomic imbalance, hyperarousal, and impaired stress recovery. In the context of trauma treatment, energy-based therapies aim to stabilize these physiological patterns and support the body’s capacity to return to baseline after stress. Rather than beginning with narrative processing alone, these approaches work bottom-up—influencing neural signaling, stress chemistry, and cellular energy production.
Some interventions use low-level electrical microcurrents or specific light wavelengths to influence brain function and mitochondrial activity. Others stimulate points on the body associated with autonomic regulation.
Examples include cranial electrical stimulation (CES), photobiomodulation, acupuncture, and meridian-based approaches. Energy psychology methods—such as Emotional Freedom Techniques (EFT) and Thought Field Therapy—combine somatic stimulation with cognitive processing, often alongside CBT or EMDR, to reduce conditioned stress responses.
When physiological regulation improves, emotional processing becomes more accessible, and therapeutic work can proceed with greater stability.
Cranial Electrical Stimulation (CES)
Cranial Electrical Stimulation (CES) is one of the most researched technological applications within energy medicine. It is a nonpharmacological intervention used for anxiety, depression, insomnia, and substance withdrawal (Kulkarni & Smith, 2001; Novakovic et al., 2011).
CES delivers a low-level pulsed microcurrent through electrodes placed on the earlobes or behind the ears, reaching subcortical structures including the hypothalamus (Ferdjallah et al., 1996). Although its precise mechanisms continue to be studied, research suggests it may influence neurotransmitter regulation—including serotonin and GABA pathways — and reduce stress-related cortisol levels (Rosch & Markov, 2004).
CES is FDA-approved for anxiety, depression, and insomnia. While research findings are mixed due to methodological variability, clinical experience suggests it may be particularly helpful for individuals with hyperarousal and sleep disturbance.
Photobiomodulation (PBM)
Photobiomodulation (PBM), also known as low-level laser or near-infrared light therapy, is another emerging intervention within energy medicine. It involves the transcranial application of non-ionizing light to support mitochondrial function.
Mitochondria produce adenosine triphosphate (ATP), the primary source of cellular energy. Trauma, PTSD, and traumatic brain injury (TBI) are increasingly associated with impaired mitochondrial function and disrupted cellular metabolism. PBM has been shown to enhance ATP production, improve cerebral blood flow, and reduce oxidative stress — mechanisms that may support neural recovery and regulation.
Clinical studies report improvements in PTSD and TBI symptoms (Lamartiniere et al., 2019) and moderate to large effects in major depressive disorder (Caldieraro & Cassano, 2019). Animal models suggest that early PBM intervention may even reduce trauma-related fear responses (Li et al., 2021).
PBM is generally well tolerated with minimal reported adverse effects. While research is still developing, its focus on restoring cellular energy aligns closely with integrative approaches to trauma recovery.
Why Energy Medicine Matters in Trauma
Trauma dysregulates the autonomic nervous system, alters stress hormone patterns, impairs sleep architecture, and disrupts mitochondrial energy production. Traditional psychotherapy addresses narrative and cognitive dimensions of trauma. Energy medicine addresses regulation and physiology.
When combined with nutritional support, targeted supplementation, movement therapy, and psychotherapeutic processing, energy-based interventions can help stabilize hyperarousal, improve sleep, enhance neuroplasticity, and increase emotional tolerance.
In trauma recovery, regulation precedes transformation. Energy medicine offers tools that work below the level of conscious thought—supporting the body’s capacity to return to balance.
Restoring Biological Coherence
Trauma disrupts the body’s internal timing systems—autonomic balance becomes unstable, stress hormones remain elevated, sleep fragments, and cellular energy production declines. While psychotherapy helps process meaning and memory, underlying biological instability can limit how much the system can tolerate at once.
Recovery follows rhythms. The nervous system must relearn how to move flexibly between activation and rest. Energy-based interventions can support this process by recalibrating stress responses, stabilizing sleep patterns, and enhancing mitochondrial function—creating conditions in which emotional work becomes more sustainable.
As biological coherence improves, resilience increases. The body becomes less reactive, more adaptive, and better able to integrate experience without becoming overwhelmed. Energy medicine is not a substitute for psychotherapy or medical care, but part of a comprehensive model that supports healing from the cellular level upward.
Without an integrative framework, trauma treatment risks managing symptoms without fully stabilizing the systems that sustain them.
These principles—nervous system recalibration, mitochondrial support, and the restoration of biological rhythm—are explored in greater depth in Rhythms of Recovery: Integrative Medicine for PTSD and Complex Trauma, where they are situated within a broader clinical model of trauma care.
References
Caldieraro, M. A., & Cassano, P. (2019). Transcranial and systemic photobiomodulation for major depressive disorder: A systematic review of efficacy, tolerability and biological mechanisms. Journal of Affective Disorders, 243, 262–273. https://doi.org/10.1016/j.jad.2018.09.048
Ferdjallah, M., Bostick, F. X., & Barr, R. E. (1996). Potential and current density distributions of cranial electrotherapy stimulation (CES) in a four-concentricspheres model. IEEE Transactions on Biomedical Engineering, 43(9), 939–943.
Kulkarni, A. D., & Smith, R. B. (2001). The use of microcurrent electrical therapy and cranial electrotherapy stimulation in pain control. Clinical Practice of Alternative Medicine, 2(2), 99–102.
Lamartiniere, R., Bergeron, R., Aung-Din, R., Bennett, M., Stephan, W., & Banas, L. (2019). Photobiomodulation treatment for brain disorders: Posttraumatic stress disorder (PTSD) and dementia. In M. R. Hamblin and Y.-Y. Huang (Eds.), Photobiomodulation in the brain: Low-level laser (light) therapy in neurology and neuroscience (pp. 589–597). Academic Press. https://doi.org/10.1016/B978-0-12-815305-5.00042-7
Li, Y., Dong, Y., Yang, L., Tucker, L., Zong, X., Brann, D., Hamblin, M. R., Vazdarjanova, A., & Zhang, Q. (2021). Photobiomodulation prevents PTSD-like memory impairments in rats. Molecular Psychiatry, 26(11), 6666–6679. https://doi.org/10.1038/s41380-021-01088-z
Novakovic, V., Sher, L., Lapidus, K. A. B., Mindes, J., Golier, J. A., & Yehuda, R. (2011). Brain stimulation in posttraumatic stress disorder. European Journal of Psychotraumatology, 2, 5609. https://doi.org/10.3402/ejpt.v2i0.5609
Rosch, P. J., & Markov, M. S. (Eds.). (2004). Bioelectromagnetic medicine. Marcel Dekker.
- Culture as Medicine: Why Trauma Must Be Healed in Cultural Context - March 27, 2026
- Integrative Energy Therapies for Trauma and Nervous System Healing - March 16, 2026
- Cooking with Spices and Herbs for Mental Health - March 6, 2026

Are You Ready to Advance Your Career?
If you want to advance your career in integrative medicine, explore my courses and certifications.