Certificación
Integrative Manual Therapies for Women’s Reproductive and Hormonal Health
An expanding body of clinical research highlights the effectiveness of manual therapies—particularly osteopathic and visceral manipulation—in improving the quality of life for women experiencing gynecological conditions. These techniques have shown promise in reducing menstrual pain, enhancing mobility, and addressing emotional well-being when traditional treatments fall short.
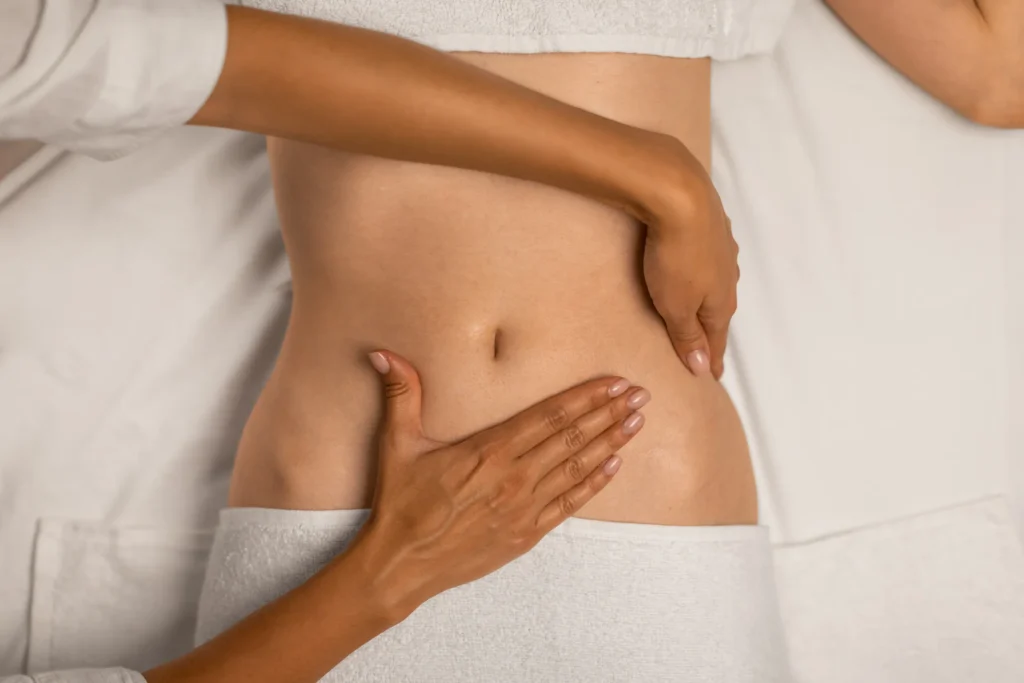
I often work with women who experience pelvic pain, endometriosis, dysmenorrhea, and hormonal imbalance in my clinical practice. These conditions extend beyond the physical body, affecting a woman’s sense of agency, comfort, and daily life. Many of my clients have tried different conventional treatments, including surgery, yet continue to seek approaches that address their pain, discomfort, mobility and the emotional challenges that accompany these chronic gynecologic conditions.
Manual therapies—including visceral manipulation, osteopathic treatment, and polarity therapy—have long been part of my integrative approach because they offer gentle, hands-on support that acknowledges the complex relationship between structure, function, and the autonomic nervous system.
Recent research suggests that these therapies may be useful in complementing gynecological care, reducing pain, improving quality of life, and helping women feel more at ease in their bodies. Below, I review five studies that explore the potential role of manual and osteopathic treatments in pelvic and reproductive health.
The first study examined the effect of osteopathic visceral manipulation on quality of life and postural stability in women with endometriosis and women with pelvic organ prolapse. Sixty women received weekly visceral manipulation sessions for five weeks. Quality-of-life scores improved significantly in both groups, with stronger results among women with endometriosis.
The second study is a systematic review that evaluated osteopathic manipulative treatment (OMT) for dysmenorrhea. OMT was associated with reductions in menstrual pain, back pain, analgesic use, and the duration of painful symptoms across ten studies. Although the techniques varied widely and no single OMT approach emerged as superior, the overall findings suggest that OMT can offer symptomatic relief.
The third study, a randomized controlled trial, examined the effectiveness of five individualized osteopathic treatments for primary dysmenorrhea. Compared with a waiting-list control group, women receiving osteopathic care experienced significant reductions in menstrual pain intensity and nearly one fewer day of pain per cycle. These improvements were observed over three menstrual cycles.
The fourth study evaluated an eight-week manual therapy protocol for women with pelvic pain related to endometriosis. Participants receiving manual therapy showed improvements in pain intensity, lumbar mobility and physical quality of life compared with participants in the placebo group. Pain improvements persisted at one- and six-month follow-ups.
The fifth study is a scoping review of available treatments and adjunctive therapies for PCOS. The authors synthesized findings from 41 studies and identified a wide range of therapeutic options. The review noted that osteopathic manipulative therapy and acupuncture decreased sympathetic tone and androgen levels.
Tags: osteopathic treatment, visceral manipulation, manual therapy, dysmenorrhea, endometriosis, pelvic pain, polycystic ovarian syndrome (PCOS), complementary medicine, non-musculoskeletal conditions, integrative women’s health
Interested in Learning More?
- Course(s): PTSD, Complex Trauma, and Traumatic Brain Injury
- Course(s): Pull the Plug on Stress: Self-Care Circuit Breaker
- Book(s): Natural Woman: Herbal Remedies for Radiant Health at Every Age and Stage of Life
Research Glossary
Research has its own vocabulary. To help you decipher research, I created a Glossary to ease the way. You may access it here: Research Glossary
Referenced Research Publications
Journal of clinical medicine
2025, enero 24
DOI: 10.3390/jcm14030767
The Effect of Osteopathic Visceral Manipulation on Quality of Life and Postural Stability in Women with Endometriosis and Women with Pelvic Organ Prolapse: A Non-Controlled Before–After Clinical Study
Abstract
Background: Visceral manipulation is a soft tissue manual work technique that originates from and is classified within the Osteopathic Manipulative Technique (OMT), focusing on the fascial tissue mobilisation of the visceral system. Manual therapy on internal organs is based on anatomy, physiology and physics.
Methods: Sixty women with endometriosis and pelvic organ prolapse, aged 41.5 ± 12.02, participated in the study. The women had manipulation therapy once a week for 5 weeks. The World Health Organisation Quality of Life BREF questionnaire and a postural stability assessment were administered before and after performing visceral manipulation.
Results: The p-value = 0.0093 obtained in the group with prolapses and the p-value = 0.0001 in the group with endometriosis indicated that the applied visceral manipulation improved the women’s quality of life. No effect of therapy was observed on postural stability.
Conclusions: Visceral manipulation improved the quality of life of both study groups of women. A significant difference was also observed when comparing the two groups for area.
Reference
Wójcik, M., Kampioni, M., Hudáková, Z., Siatkowski, I., Kędzia, W., & Jarząbek-Bielecka, G. (2025). The Effect of Osteopathic Visceral Manipulation on Quality of Life and Postural Stability in Women with Endometriosis and Women with Pelvic Organ Prolapse: A Non-Controlled Before-After Clinical Study. Journal of clinical medicine, 14(3), 767. https://doi.org/10.3390/jcm14030767
Curēus
2024, enero 23
DOI: 10.7759/cureus.52794
Osteopathic Manipulative Treatment in Dysmenorrhea: A Systematic Review
Abstract
The majority of women experience dysmenorrhea during their lifetime. The current standard-of-care treatment consists of nonsteroidal anti-inflammatory drugs, oral contraceptive pills, or intrauterine devices. Osteopathic manipulative treatment (OMT) is a beneficial tool for improving non-musculoskeletal (non-MSK) conditions such as migraines, gastroesophageal reflux disease (GERD), and anxiety. OMT should be utilized to improve other non-MSK conditions, such as dysmenorrhea. The current review aims to evaluate the effects of OMT in women with dysmenorrhea. An extensive search was conducted in Cumulative Index to Nursing and Allied Health Literature (CINAHL), MEDLINE, Biomedical Reference Collection: Comprehensive, and Nursing & Allied Health Collection: Comprehensive from inception to June 2022. Studies evaluating the use of OMT in patients with dysmenorrhea were included, while editorial/opinion articles were excluded. Three independent reviewers evaluated the studies. Ten studies evaluating the use of OMT in patients with dysmenorrhea were included. Overall, OMT was shown to provide relief of symptoms, including back and menstrual pain; however, there was no guideline on which OMT techniques are the most successful. Numerous positive effects were found, including a reduction in the duration of pain, reduction of pain intensity, and reduction of analgesic use. However, the low number of studies supports the need for further investigations. Dysmenorrhea patients could benefit from a prospective randomized controlled trial targeting spinal facilitation and viscerosomatic reflexes to decrease pain duration, pain intensity, and analgesic use. Non-MSK-focused OMT has a large body of mostly anecdotal evidence for relief of conditions such as migraine, GERD, and anxiety. It has helped when traditional standards of care have failed. Non-MSK-focused OMT research represents a relatively untouched field of research that can have a profound and positive global impact, particularly in areas with poor income/healthcare access.
Reference
Bonner, P. E., Paul, H. A., & Mehra, R. S. (2024). Osteopathic Manipulative Treatment in Dysmenorrhea: A Systematic Review. Cureus, 16(1), e52794. https://doi.org/10.7759/cureus.52794
Journal of bodywork and movement therapies
2025, enero 25
DOI: 10.1016/j.jbmt.2025.01.041
Effectiveness of osteopathic treatment in women with primary dysmenorrhea: A randomised controlled trial
Abstract
Effectiveness of five osteopathic treatments in patients with primary dysmenorrhea. Two-centre randomised controlled trial with women in northern Germany of ages between 12 and 53 years with medically-diagnosed primary dysmenorrhea. Treatments were allocated by an external institution using computer generated tables. Neither the therapists nor the participants were blinded. Five individual, findings-based osteopathic treatments (black box method) and follow-up time versus waiting-list. Main outcome measures Intensity and duration of menstrual pain with Numeric Rating Scale. 72 individuals were randomised to treatment group (n = 35) or control group (n = 35) (drop-outs n = 2). The inter-group comparison demonstrated a statistically significant decrease in pain intensity (NRS score: difference in mean value 1.7; 95% CI: 0.9 to 2.6; p < 0.005). In the inter-group comparison, the number of days in pain decreased in a statistically significant way by the mean value of 0.8 days (95% CI: -2 to 0.4; p = 0.04). Five osteopathic treatments over a period of three menstrual cycles may be effective in relieving the duration and intensity of menstrual pain in women with primary dysmenorrhea. Additional and larger studies using sham control group interventions are needed to confirm the current results.
Reference
Plathner, M., & Wolf, L. (2025). Effectiveness of osteopathic treatment in women with primary dysmenorrhea: A randomised controlled trial. Journal of bodywork and movement therapies, 42, 684–692. https://doi.org/10.1016/j.jbmt.2025.01.041
Journal of clinical medicine
2023, mayo 06
DOI: 10.3390/jcm12093310
Effectiveness of a Manual Therapy Protocol in Women with Pelvic Pain Due to Endometriosis: A Randomized Clinical Trial
Abstract
A randomized controlled trial was carried out to assess the effectiveness of a manual therapy protocol in terms of the clinical characteristics, quality of life, and emotional condition of the women with endometriosis-related pelvic pain. Forty-one women (mean age of 36.10 (6.97) years) with pelvic pain due to endometriosis were randomly divided into (i) a manual therapy group (MTG) (n = 21) and (ii) a placebo group (PG) (n = 20). Both groups received an 8-week intervention. Pain, lumbar mobility, endometriosis health profile, quality of life, depression and anxiety levels, and the patient’s perception of change were assessed before (T0) and after (T1) the intervention, as well as at a one-month follow-up (T2) and a six-month follow-up (T3). The MTG significantly improved pain intensity, powerlessness, lumbar mobility, and physical quality of life at T1 (p < 0.05). The results were maintained for pain intensity at T2 and T3. In addition, both the MTG and PG improved emotional wellbeing at T1 (p < 0.05). Neither group improved in terms of social support, self-image, and depression and anxiety levels after the intervention (p > 0.05). In conclusion, manual therapy may be an excellent complement to the gynecological treatment of endometriosis-related pelvic pain by alleviating pain and improving women’s endometriosis health profile and physical quality of life.
Reference
Muñoz-Gómez, E., Alcaraz-Martínez, A. M., Mollà-Casanova, S., Sempere-Rubio, N., Aguilar-Rodríguez, M., Serra-Añó, P., & Inglés, M. (2023). Effectiveness of a Manual Therapy Protocol in Women with Pelvic Pain Due to Endometriosis: A Randomized Clinical Trial. Journal of clinical medicine, 12(9), 3310. https://doi.org/10.3390/jcm12093310
Curēus
2024, septiembre 30
DOI: 10.7759/cureus.70501
Available Treatments and Adjunctive Therapies for Polycystic Ovarian Syndrome (PCOS) Patients of Reproductive Age: A Scoping Review
Abstract
Polycystic ovarian syndrome (PCOS) impacts the health of women worldwide. It is a condition consisting of dysfunctional cystic ovaries resulting in hormonal imbalance. Many women have symptoms such as infertility, increased production of androgens, and insulin resistance. Barriers to effective treatment of PCOS include issues such as delays in diagnosis and inconsistencies in treatment plans among physicians. Despite the current use of available medications to decrease symptomatology, women with PCOS continue to report a decreased quality of life. Using the electronic databases PubMed, Cumulative Index to Nursing and Allied Health Literature (CINAHL), and ScienceDirect, a scoping review was conducted on the globally available treatments for PCOS. After applying pre-determined inclusion criteria, 41 studies were included in this scoping review. The literature on the available treatments for PCOS revealed a wide range of therapeutics with evidence of reduction of symptoms and/or improvement in fertility status and pathological processes such as insulin resistance, hormone imbalance, obesity, inflammation, and infertility. Dozens of treatment options for PCOS have been identified, including new medications and modifications to existing treatment regimens. The hormonal drug Fezolinetant demonstrated effective suppression of hyperandrogenism. Drugs used to treat diabetes, such as Liraglutide, were found effective for weight loss. Green cardamom, cinnamon, and other supplements proved effective in treating metabolic dysfunction. Alternative approaches, such as osteopathic manipulative therapy and acupuncture, decreased sympathetic tone and androgen levels. This review provides a succinct overview of PCOS therapies that can be used by those with PCOS and their physicians everywhere. With a better understanding of their options, women with PCOS can become more involved in the decision-making process to improve their health. More research is needed on novel therapies that aim to reduce the primary pathogenesis of PCOS.
Reference
Cochran, L., Nadolny, R., Garcia, K., Kluglein, K. A., Yagoda, A., Gandhi, P., Dressel, J., Prol, B., Peralta, R., Shipp, A., & Costin, J. M. (2024). Available Treatments and Adjunctive Therapies for Polycystic Ovarian Syndrome (PCOS) Patients of Reproductive Age: A Scoping Review. Cureus, 16(9), e70501. https://doi.org/10.7759/cureus.70501